Each year, the Royal Australian College of General Practitioners (RACGP), conducts a range of surveys and collates data from nationwide sources to generate an insight into the state of general practice in Australia. From this, the annual Health of the Nation report is produced and published.
Given the tumultuous events of the past several years in Australia, beginning with a spate of bushfires in late 2019, followed by the COVID-19 pandemic from early 2020 to the present day, the RACGP 2020 Health of the Nation report has presented some stark differences when compared to prior editions.
This article summarises some of the findings from the 2020 Health of the Nation report, primarily those relating to current and emerging issues, telehealth, the funding of Australian general practice care, and the business and economics of a general practice.
Common Health Presentations in General Practice
Unsurprisingly, issues relating to the 2019-2020 bushfires and the ongoing COVID-19 pandemic were represented heavily when considering common reasons for presenting to GPs in 2020. Psychological issues including depression and anxiety remained the most prevalent, with 64% of surveyed GPs listing psychological issues among their top three most common reasons for patients presenting.
Preventive care, primarily comprised of vaccinations and health screenings, rose to the second most prevalent reason for presenting to a GP. This was largely due to the government drive to encourage early vaccinations for things like the seasonal flu to avoid heaping more stress onto the healthcare system during the pandemic. It’s interesting to note that while vaccinations increased, preventive health screenings dropped, likely as patients were not presenting for usual care among COVID-19 directives.
The Mental Health Impact of Natural Disasters
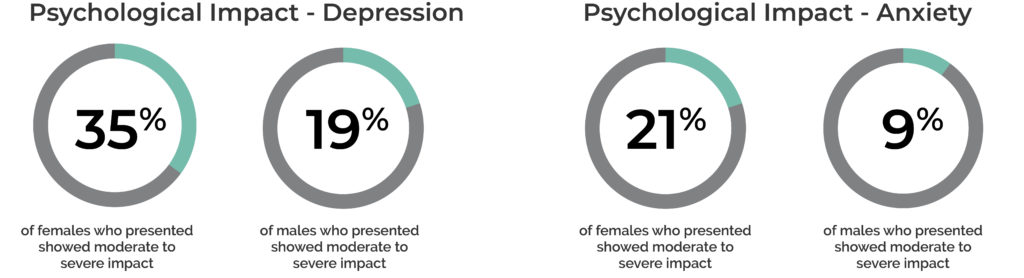
For the fourth year running, the RACGP 2020 Health of the Nation report has listed psychological issues as the single most prevalent reason that Australians are presenting to GPs.
While the COVID-19 pandemic has impacted the entirety of the Australian population to some degree, young Australians have been impacted most heavily, with female patients being disproportionately affected within that subset.
But it is not just patients being negatively affected – healthcare workers were similarly affected. While 43% of GPs reported no impact to their wellbeing, 57% reported a negative change to their wellbeing with regards to either physical health, being able to maintain a healthy work-life balance or managing their mental health.
This is of particular concern, as GPs have, for the past several years, ranked managing their own wellbeing as one of the top three challenges for being able to provide consistent, high-quality patient care.
Issues Requiring Policy Action
When it comes to policy issues that GPs believe require action, MBS patient rebates are the most significant area of priority for the fourth consecutive year with more than 40% of surveyed GPs placing it in their top three issues for policy action.
Consideration for mental health services remains the second most identified area for Australian Government priority, while a focus on creating new funding models for primary healthcare rounds out the top three most significant issues.
However, the priorities of GPs working in Aboriginal Medical Services did vary slightly. For GPs working in these communities, social and cultural determinants of health equity and equality held particular concern, with 33% and 31% respectively noting these issues in their top two policy concerns.
A Critical Issue in Focus - Pandemic Response
When it came to considering the Australian Government’s response to the pandemic, the survey showed mixed opinions.
On one hand, many GPs supported the government’s initial response, with one in two GPs labeling the response either ‘good’ or ‘very good’ with regards to ensuring the safety of GPs and their Practice teams.
GPs were also quick to acknowledge that amid a pandemic, the need for telehealth was identified quickly and acted upon – with the government quickly providing funding to support the model of care.
However, many GPs also noted that much more could have been done in the early stages of the pandemic and throughout its progression to support frontline healthcare workers. A particular challenge and area of concern was accessing personal protective equipment (PPE). Eight out of 10 GPs surveyed believed that the government could have done much better in providing Practices with PPE when they needed it most.
Of the many challenges faced by GPs during the COVID-19 pandemic, the inability to provide their usual standard of care to patients ranked the most highly, with the aforementioned lack of access to PPE following closely behind, with a notable number of GPs citing the constantly changing MBS rules as a cause of concern also.
Perhaps the most interesting statistic to consider when looking at the pandemic response holistically is the percentage of Australians that visited a GP. During 2019-2020, 87.4% of Australians visited a GP, which was the lowest rate seen in the country since 2014-2015. This is likely due to a significantly decreased number of patients presenting for usual care while they were being encouraged to isolate at home, or socially distance under COVID-19 directives.
A Fast-Tracked Adoption of Telehealth
When social distancing measures and stay-at-home mandates were implemented, telehealth quickly became the standard by which GPs would continue to be able to offer consultations while still being able to protect themselves, their patients and Practice staff.
Prior to the COVID-19 pandemic, only 17% of GPs surveyed had used telehealth to deliver a consultation – 4% via video, and 13% over the phone. During the pandemic however, 30% of GPs conducted at least one telehealth consultation over video, and 96% conducted a consultation over the phone.
When asked about their thoughts on the initiative, 67% of GPs reported a positive change in their attitude towards telehealth, with only 10% noting a negative shift in attitude.
Those that felt positively about it noted that telehealth allowed them to see their patients more regularly and in a timely manner, which often led to patients discussing health concerns as they arose, rather than ‘saving them all up’ and attempting to fit each concern into a single consult. In addition, GPs noticed an increased feeling of safety and security in patients being able to consult with them in their own home. This was of particular benefit for mental health consultations and some forms of counselling.
Among those who felt negatively towards telehealth, the primary reason was that they felt telehealth presented limitations to the provision of patient care, and that telehealth should complement, not replace, face to face consultations.
7 out of 10 GPs believe that a continuation of telehealth consultations post-pandemic is possible, and it would continue to support patient access to high-quality care in general Practice. However, many noted that telehealth should only be made available to patients already known to the Practice and should only be available for specific types of consults; repeat scripts, discussing uncomplicated test results, some forms of counselling, and referrals.
Government Contribution to Patient Services
Australian government contributions to patient services continues to be an area of concern for general Practice. While most patient care in Australia is being delivered in the general Practice sector, the overwhelming majority of government healthcare expenditure is in hospitals.
In 2017-18, state and federal governments spent approximately $52 million in the hospital sector, while unreferred medical services (which is primarily general Practice), received a little over $11 million, with almost the entire expenditure coming solely from the federal government.
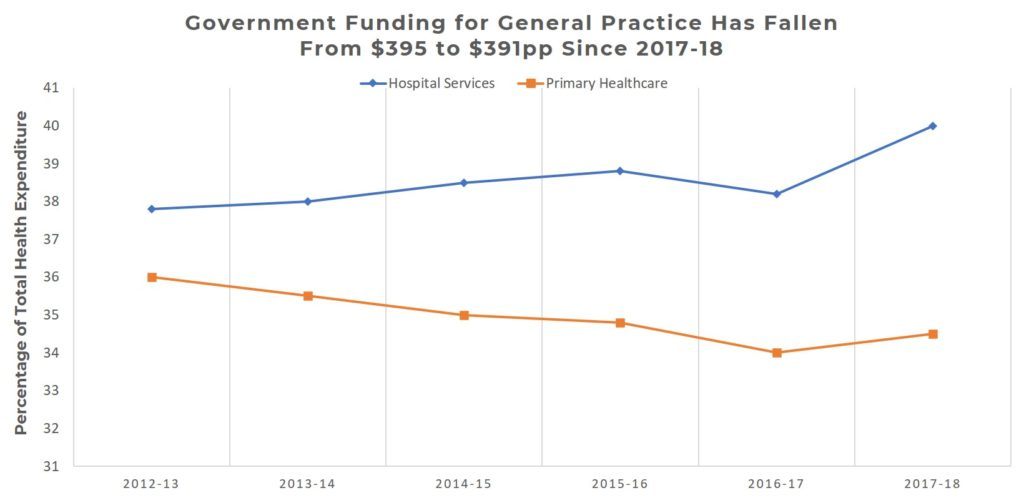
Across both state and federal governments, the total expenditure on general Practice is approximately 7.5% of the nation’s total health expenditure.
The Australian government’s expenditure on healthcare, as a share of our gross domestic product (GDP), is lower than almost all other developed countries with a similar primary care focused system.
Trends in General Practice Billing
The 2020 RACGP Health of the Nation report showed the following bulk billing trends in 2019-2020:
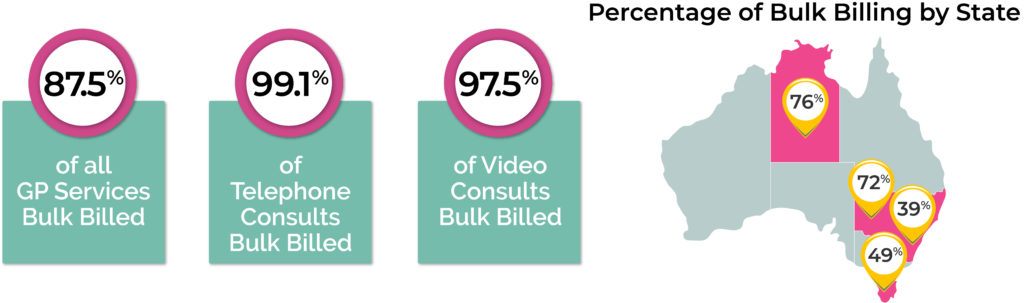
The report did note, however, that patients may receive multiple services when visiting their GP, and that some of those services may be bulk billed, while others are billed privately.
Nationally, the proportion of patients who have all GP services bulk billed is rising, but in several states the rate is in decline. It is also interesting to note that while the number of bulk billed services has increased year on year, each year the rate of increase slows further.
Business and Income Challenges in General Practice
General Practice as a business is a key part of the Australian healthcare sector, worth over $13b annually to the Australian economy, and employing more than 100,000 people nationwide.
When consulting GP Practice owners about the most common challenges they face, respondents nearly unanimously agreed that maintaining a healthy work-life balance, maintaining a steady income, and sourcing and retaining quality staff were at the top of their list of concerns.
GP Practice owners working in regional, rural, or remote areas were still concerned with managing a work-life balance and steady income but are comparatively more concerned with ensuring the ongoing delivery of high-quality care to patients from disadvantaged backgrounds.
GPs and Practice owners noted that at a time when the country needed their services most, many were faced with a lack of job security. In a survey conducted in May of 2020, 71% of GPs reported that their income was lower than the same time the previous year, with 25% of those reporting a much lower income. Only 5% of GPs reported a higher income than the previous year.
When asked for their thoughts on the main contributing factors for the reduction in income, 83% cited fewer patients presenting for care among stay-at-home directives. 70% also indicated that while telehealth consultations did allow patients to still present to their GP, the requirement to bulk bill these telehealth consultations contributed significantly to a reduction in income. Approximately 50% of GPs surveyed agreed that the removal of mandatory bulk billing of telehealth services would improve the viability and sustainability of their Practice.
There were a range of other reasons cited for reduced income revenue – these included reduced rental income, reduced work hours, changing circumstances and generally increased demands in response to the COVID-19 pandemic.
Practice Ownership
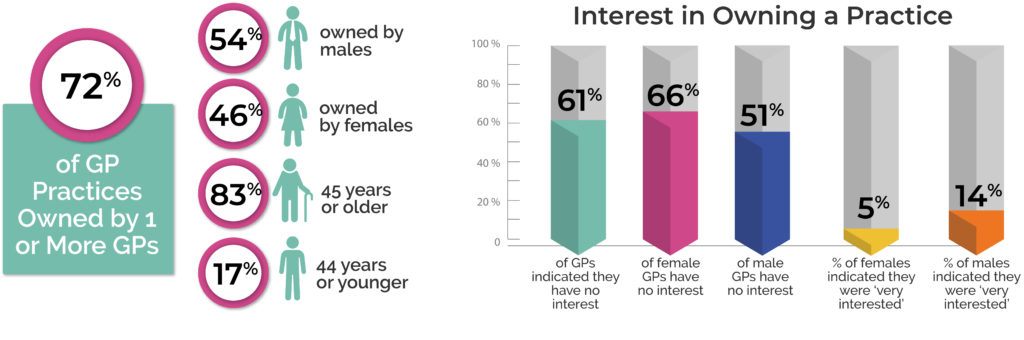
The trend in Australian Practice ownership continues to shift towards more heavily towards multi-partner and corporate arrangements. Broadly speaking however, GP interest in owning a Practice is relatively low, even more so amongst women. Just over a quarter of Practices operate in conjunction with other businesses, with 28% of GPs surveyed reporting that their Practice was networked with another site, often sharing human resources, payroll, marketing, or clinical governance arrangements.
The 2020 RACGP Health of the Nation Report in Summary
The RACGP Health of the Nation report is an incredibly insightful, thorough report for which we have only just scratched the surface. However, even this brief look has managed to outline some interesting data points, both new and recurring, that have surfaced over the past 2 years.
Given recent and ongoing tumultuous events, many of which disproportionately affect the healthcare sector and in particular GPs, the 2021 Health of the Nation report should shed some light on whether many of these trends are anomalies, or whether they will begin to evolve and embed themselves into what we now consider the ‘new normal’.
The RACGP Health of the Nation report for 2020, along with previous editions, are available to read in full here.
Authored by:
Louis Valenti
Marketing Specialist at Best Practice Software
Explore our range of news and training resources:
Bp Learning Video Library | Bp Learning Training Options | Bp Newsroom Blog
Subscribe to Our Newsletters | Bp Learning Webinars