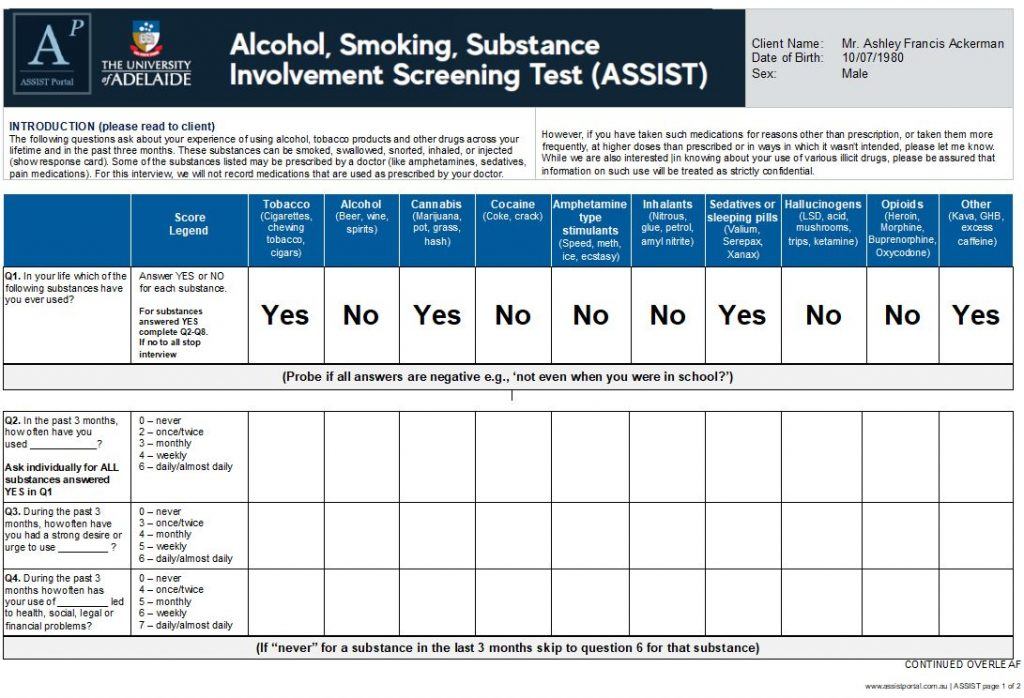
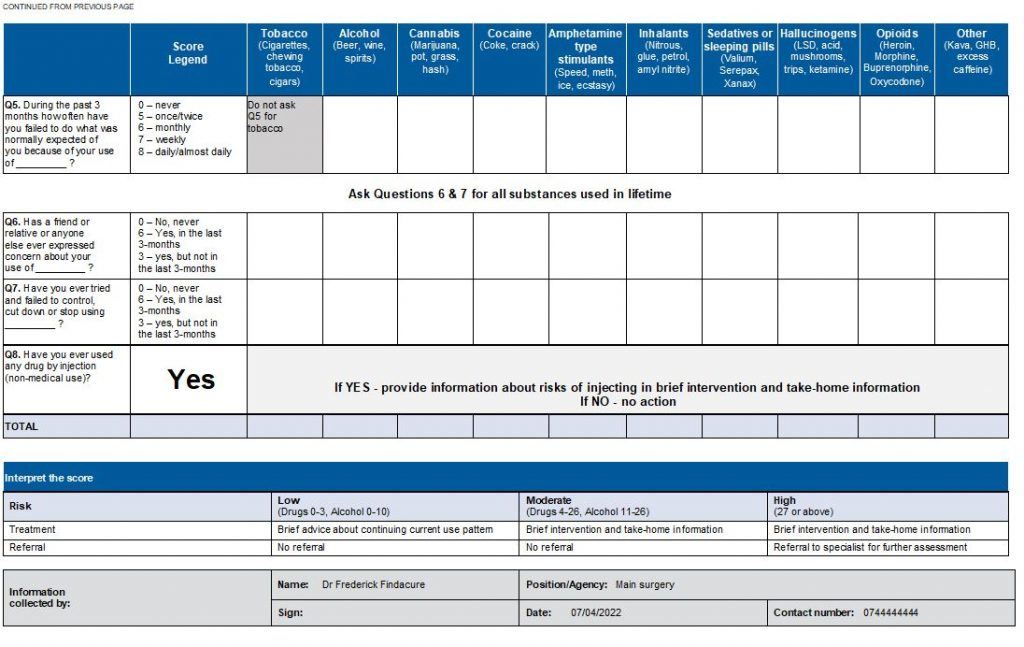
In Australia, all doctors and nurse practitioners can legally prescribe medicinal cannabis to their patients with specific medical conditions through the Therapeutic Goods Administration (TGA) Special Access Scheme. To date, there have been over 220 conditions approved by the TGA. Recently there have been significant improvements to the application process when prescribing medical cannabis to improve patient access and reduce the administrative burden on you as the prescriber.
The below information has been taken from the TGA website:
“If you determine that an ‘unapproved’ medicinal cannabis product is clinically suitable for your patient, there are four pathways through which your patient can access the product with your prescription.”
Authorised Prescriber - 'Established History of Use' Pathway
Medical practitioners can apply to become Authorised Prescribers of specified medicinal cannabis products without the need for approval from a Human Research Ethics Committee or endorsement from a specialist college.
Medicinal cannabis products and indications deemed by the TGA to have established history of use are specified in the list of medicines with an established history of use.
Authorised Prescriber - Standard Pathway
Medical practitioners can apply to become Authorised Prescribers of medicinal cannabis products not included in the list of medicines with an established history of use via the standard pathway. This pathway requires approval from a Human Research Ethics Committee, or endorsement from a specialist college before applying to the TGA.
SAS Category A Notification Pathway
Medicinal cannabis products supplied via the SAS Category A pathway must be imported on a patient-by-patient basis with permission from the Office of Drug Control (ODC).
SAS Category B Application Pathway
The SAS Category B pathway is an application pathway available to prescribing healthcare practitioners including Medical Practitioners and Nurse Practitioners. When applying to access an unapproved medicinal cannabis product on behalf of a patient under the SAS Category B pathway, prescribers must provide a clinical justification. The justification should include the seriousness of the patient’s condition, consideration for the use of medicines that are included in the ARTG and the potential risks and benefits of using the proposed unapproved medicine.
There are no restrictions on the medical conditions for which a prescriber may apply via the SAS to access an unapproved medicinal cannabis product for their patient, provided the prescriber has the appropriate knowledge on the condition being treated and on the medicinal cannabis product they wish to prescribe.
Reporting
MedReleaf Authorised Prescriber Now Available in the Bp Premier Reporting Tool
The MedReleaf Authorised Prescriber 6-Monthly Report is to support prescribing doctors who are authorised prescribers for unregistered medical cannabis products. Authorised prescribers for unregistered medical cannabis products need to report the number of new patients commenced on treatment, and number of patients continued on treatment (for longer than 6 months), for each product to the Therapeutic Goods Administration.
This report takes the stress out of keeping track of patient numbers throughout the reporting period. A simple report generation saves the doctor and clinic ample administrative work.
To learn more on the TGA Reporting Tool please visit: MedReleaf 6 monthly TGA reporting
Learning
MedReleaf Prescriber Program
MedReleaf Australia’s prescriber program is available to all doctors, providing access to training and education for the doctor to confidently assess, advise, prescribe and treat patients with medical cannabis.
Peer-to-peer workshops, educational webinars and further clinical material are available through registering to access MedReleaf’s online training and education portal, available here.

Explore our range of news and training resources:
Bp Learning Video Library | Bp Learning Training Options | Bp Newsroom Blog
Subscribe to Our Newsletters | Bp Learning Webinars